Taking a Pulse: Clinician Poll on Migrant and Immigrant Patient Care
“I find that my patients are living under constant fear and stress. They express to me that they no longer feel safe or welcomed in their communities. Many families are becoming more isolated and their lives are confined to work and home. They are less likely to be engaged in their communities and this is leading to higher levels of stress and anxiety, which is exacerbating their other chronic conditions. ” --Physician Poll Respondent, February 2018
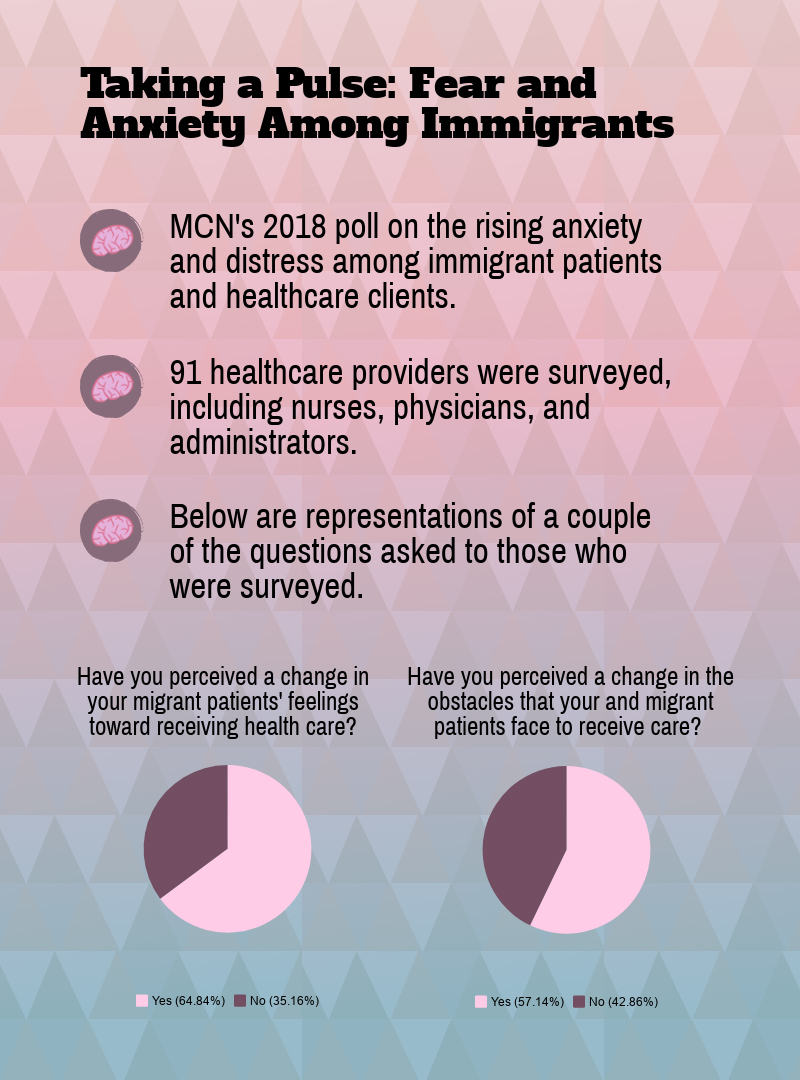
A new poll of 91 health care providers and clinical staff found that 65 percent of respondents have seen a change in the last year in immigrant or migrant patients’ attitudes or feelings toward health care access. Most of the respondents who have seen a change cited an increase in fear among their patients that drives them to avoid care. A shift in immigration policies and the resulting changes in local communities (from increased ICE presence to negative community perceptions and rhetoric around immigrants) are called out as primary drivers of fear. Slightly fewer respondents (57 percent) have seen a change in the obstacles that immigrant or migrant patients face to receive care. Many respondents reported a wide range of long-standing common obstacles -- language barriers, limited transportation options, limited clinic open times, lack of access to specialists -- now compounded upon by fears related to immigration.
This new poll, taken by Migrant Clinicians Network in January and February 2018, reflected the experiences of clinical staff from 26 states across the country. Respondents came from every corner of the clinic; occupations listed include Physician, Executive Director, Dental Assistant, Outreach Specialist, Therapist, Community Health Worker, Registered Nurse, and 24 other occupations. The poll follows up on MCN’s 2017 poll, in which 63 percent of respondents indicated that immigrant and mobile patients’ attitudes and feelings toward health care access had changed.

“As our clinical colleagues are reporting from all over the country, fear continues to compromise their best efforts to create true access to primary care services. Feelings of despair and fatigue prevail on both sides; patient and provider,” noted Karen Mountain, MBA, MSN, RN, Chief Executive Officer for MCN. “We dream of a day when they can have the ability to create a safe culture of care for our patients as we continue to deal with the aftermath of ‘too little, too late.’”
Many respondents cited national affairs like changes in immigration and health care policies and strong rhetoric around immigration as the reasons for a change in perceived access to care, while others pointed to local raids by the US Immigration and Customs Enforcement (ICE) that discouraged people from getting care when they needed it and affect the mental health of both those targeted and the immigrant and migrant communities as a whole.
Immigration enforcement, policy, and rhetoric aren’t the only immigration-related fears that respondents highlighted. Comments like “openly racist community confrontations,” “documented patients harassing Latinx patients in the waiting room,” “University hospital now refuses to give charity care to immigrants with a visa” demonstrate that local communities’ responses to immigration concerns can add to patients’ reluctance to seek care.
Almost 30 percent of respondents found that community perception of their work has changed. One respondent noted, “we see more people trusting less, asking if we share information.” Some respondents felt that community perception of the clinic or hospital had changed for the better, with positive responses to outreach programs and greater support from local communities.
Similarly, at least two respondents felt that perception of access to care had changed for the better, crediting health centers’ education efforts and extension of clinic hours for serving patients better. Another noted that, little by little, patients are losing their fear.
Wording of the poll led to mixed responses. One respondent noted that, in the last year, there hasn’t been a significant change -- that fear and anxiety have now been discouraging patients for well over a year.
The poll’s 2017 responses were very similar to this year’s responses. In 2017, almost 63 percent of respondents perceived a change in immigrant and mobile patients’ attitudes and feelings toward health care access, while 48 percent perceived a change in the obstacles that patients face to receive care. Only 27 percent believe that community perception of their work had changed.
Contact Migrant Clinicians Network about this poll: chutkins-seda@migrantclinician.org.
Like what you see? Amplify our collective voice with a contribution.
Got some good news to share? Contact us on our social media pages above.
Return to the main blog page or sign up for blog updates here.
- Log in to post comments






