Statement: Community Health Workers, Outreach & Education Must Be Front & Center to Support Immigrants & Migrants When COVID-19 Vaccination Arrives
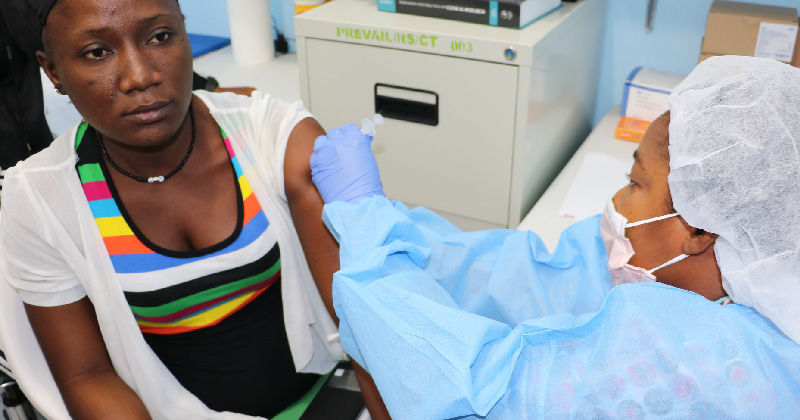
[Editor’s Note: Last week, Migrant Clinicians Network’s Chief Executive Officer, Karen Mountain, MBA, MSN, RN, spoke during the public comment session to the National Academies of Sciences, Engineering, and Medicine on the National Academies’ Discussion Draft of the Preliminary Framework for Equitable Allocation of COVID-19 Vaccine. Here are Mountain’s comments. A video of the entire five-hour session is now available here -- Mountain comes in at about hour 3:35.]
We thank the Committee for the opportunity to express our strong support of prioritizing immigrants and migrant workers and their families through enhanced vaccination programs at community health centers and using Community Health Workers for outreach and education. Migrant Clinicians Network (MCN) is a non-profit organization that creates practical solutions at the intersection of vulnerability, migration and health. Since 1984, MCN has addressed the social determinants of health among underserved immigrant communities with an emphasis on workers, families and children.
Over the last 36 years, our organization has grown to serve constituents globally, providing accredited training and technical assistance to the clinical workforce and developing culturally appropriate resources and programming. MCN has extensive experience in program design; implementation and evaluation; grants management; and educational materials development. This experience extends to both childhood and adult vaccination, in particular vaccine hesitancy for annual influenza and HPV.
The clinicians we serve and support provide safety-net primary care and widespread outreach to the most vulnerable, through community health centers and other health promoting agencies. Across the US and Puerto Rico, we have engaged with community-based, participatory educational outreach that serves predominantly Latinx and African American populations who have sustained the greatest harm from COVID -19. For example, MCN partners with the Ventanilla de Salud (VdS) program in the 50 geographically dispersed Mexican consulates in the US to connect low-wage, high-risk, mobile working populations with health promotion and care services.
COVID-19 has made long-standing underlying health inequities into front page news, as “essential” workers hit barrier after barrier to stay safe and get care when needed. Much of MCN’s work in 2020 has pivoted toward protecting these populations from COVID-19 and reducing health inequities that the virus has amplified.
Other pathogens besides SARS-CoV-2 can cause fevers, breathing difficulties, cough, and a myriad of symptoms which can be difficult to diagnose. These pathogens can have significant impact on populations already experiencing a disparate burden of chronic diseases. MCN recommends an enhanced, coordinated vaccination program for influenza and pneumonia this fall, preceding the development of an effective vaccine for SARS -CoV-2. This can minimize risk against mortality from influenza, pneumococcal pneumonia, bacteremia, and meningitis. Additionally, MCN is focused on creating and bolstering the networks that can mobilize within communities when a proven, safe and effective COVID-19 vaccine becomes available. Our approach will build trust and develop networks of communication and partnerships designed to reach the most vulnerable.
- The roll-out of a COVID-19 vaccine comes with lots of concerns. Generally, the most vulnerable populations who would best benefit from a functional vaccine are also the populations that have been grossly mistreated historically during vaccine trials or forced into medical procedures without consent.
- We must recognize and address this tragic racist past in our shared medical history if we are to adequately prepare the way for vaccine acceptance.
- We must continue our concerted outreach efforts, but that will not be enough.
- We must address widespread lack of health literacy.
- We must confront the spread of health misinformation online.
- We must recognize how social factors influence health – and begin to address those social factors.
We must meaningfully re-evaluate and rebuild the social and health care structures that negatively impact the health and well-being of patients. Finally, and critically, health equity must be a national priority.
Like what you see? Amplify our collective voice with a contribution.
Got some good news to share? Contact us on our social media pages above.
Return to the main blog page or sign up for blog updates here.
- Log in to post comments